LISTEN TO THIS ARTICLE:
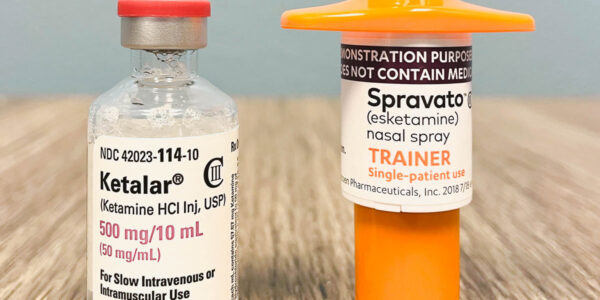
A slew of headlines made the rounds this past week concerning the link between serotonin and depression. The study, “The serotonin theory of depression: a systematic umbrella review of the evidence,” looked at research surrounding this relationship. The reason for the bevy of media coverage is that the study concludes with seemingly powerful statements:
“[T]here is no convincing evidence that depression is associated with, or caused by, lower serotonin concentrations or activity. This review suggests that the huge research effort based on the serotonin hypothesis has not produced convincing evidence of a biochemical basis to depression… We suggest it is time to acknowledge that the serotonin theory of depression is not empirically substantiated.”
The authors of the study go on to doubt the efficacy of antidepressant medications and just barely stop short of encouraging readers to stop taking prescribed medications. These are some audacious claims about a complex topic, so let’s break it down.
What is the “serotonin hypothesis”?
The “serotonin theory of depression” and “serotonin hypothesis” refer to what has historically also been called the “monoamine hypothesis” or “biological theory of depression.” This explanation originated over 50 years ago and proposed that the biological cause of depression was from a lack of brain chemicals like serotonin, dopamine, or norepinephrine.
What this review fails to mention is that the “serotonin hypothesis” has not been widely accepted as the only potential cause of depression since the 1990s. Admittedly, this explanation was and still is frequently used when describing the causes of depression for patients. People with depression often experience guilt and blame themselves for how they are feeling. The biological reasoning can help depressed people feel less like their emotions are their fault.
The biopsychosocial view
Today (and for the past two decades), the “biopsychosocial” view is the most widely accepted model for understanding depression. This concept provides a more holistic view of mental health issues. It takes input from multiple levels, from the actions of molecules in the brain all the way up to an individual’s emotions and their social interactions. Mental illness is more than just brain biochemistry. It’s emotions, experiences, and relationships. It’s incredibly complex, and we’ve known and treated it as such for many years now.
Overly simplistic conclusions
In light of this, you can see that the problem with this research review is that it draws simplistic conclusions. This study essentially equates serotonin deficiency with depression, but as we just discussed, there is so much more to it than that. Just because a drug increases the level of a certain chemical to treat a disease does not mean that the disease is caused solely by a deficiency of that chemical. Furthermore, not understanding the exact mechanism by which a drug helps people does not make it any less effective. This is true for many medications, psychiatric and otherwise.
No acknowledged limitations or conflicts
Almost every scientific study will conclude with two sections. One acknowledges the study’s potential weaknesses and another discloses any possible conflicts of interest for the study’s authors. This review disconcertingly contains neither, and that’s a red flag.
While the authors called this a “comprehensive review of… research,” it actually only looked at 17 studies. Upon their initial search for relevant studies, the authors found 360 published pieces. However, they excluded 315 of them early on and continued pairing further until only 17 remained. That seems an awfully low number of studies to use to draw such fantastic conclusions.
Suspicious motives
Another issue the authors fail to mention is that the lead author of this study, Dr. Joanna Moncrieff, has made a career out of questioning the biological model of psychiatric illness. She has written several books on the topic. They include titles like The Myth of the Chemical Cure: a critique of psychiatric drug treatment and The Bitterest Pills: the troubling story of antipsychotic drugs.
Dr. Moncrieff follows in the footsteps of Thomas Szasz, the founder of the “anti-psychiatry” movement who denied the existence of mental illness. Szasz worked with the Church of Scientology to create the Citizen’s Commission on Human Rights (CCHR), a group which denounces psychiatry and medical treatment for mental illness. This organization has touted many of Moncrieff’s other claims, most of which doubt the effectiveness of psychiatric treatments. Her assertions frequently seek to subvert established psychiatric principles without telling the whole story. Whether this should call into question the validity of this study I will leave to you to decide.
What to make of it?
Whatever your takeaway from this, please know that the link between serotonin and depression is not a black-and-white, all-or-nothing situation. Depression and all other psychiatric illness are extremely multifaceted, involving not only brain chemistry, but also social settings and complex psychology. With this in mind, no one should rely on any single study to prove or disprove something like this. Unfortunately, mass media frequently fails to report accurately on studies that make these audacious claims. They are not a good source of medical information and advice. The best source for that is your doctor or therapist. You can also explore potential depression symptoms in our symptom checker.


 Learn
Learn Read Stories
Read Stories Get News
Get News Find Help
Find Help
 Share
Share
 Share
Share
 Share
Share
 Share
Share