LISTEN TO THIS ARTICLE:
Childbirth can be traumatic. The impact of birth trauma ranges from minimal to devastating. How we heal and survive that trauma is as unique as our personalities. Meeting women’s mental health needs after a traumatic birth is essential for mothers’ healing and their families’ life-long emotional well-being.
What is birth trauma?
“Birth trauma” is an injury to either a mom or baby during delivery. It includes the emotional and psychological shock experienced by a mother during pregnancy, birth, or after delivery. Trauma with emotional consequences can happen at many points along the pregnancy journey. These include infertility treatment, miscarriage, an elective termination, or stillbirth.
Birth trauma covers the range of emotions experienced by a mom in response to the perception that either her life or her baby’s life is in danger. More severe forms of trauma are diagnosed as postpartum traumatic stress disorder. (“Postpartum” means “after childbirth.”) Not all survivors of birth trauma develop PTSD. However, if a woman experiences her birth as traumatic, she is also at greater risk for postpartum depression.
More common than you think
It’s no longer a question whether childbirth can be traumatic or, more specifically, whether birthing people can end up with post-traumatic stress disorder. -Lynne McIntyre, LCSW, Mammha Chief Maternal Health Advisor
Between a quarter and a third of women experience a traumatic birth, though not all develop PTSD. In one study of almost 500 women, one out of every three women had a traumatic birthing experience, and just as many reported at least three clinical symptoms of PTSD.
Approximately one out of every 20 women experience PTSD after delivery. Long-term effects of not healing psychologically after traumatic childbirth can include attachment and parenting difficulties.
What are the symptoms of birth trauma and postpartum PTSD?
Birth trauma has four main symptoms, and they overlap quite a bit with the symptoms of PTSD.
- Re-experiencing: People relive the traumatic event in the form of flashbacks, nightmares, or intrusive memories. This causes increased anxiety and panic attacks.
- Avoidance: People shy away from any reminders of the trauma, such as avoiding meeting other women with new babies.
- Hypervigilance: Women feel perpetually alert, irritable, and jumpy. They worry that something terrible is going to happen to baby.
- Depression: People can feel guilty and blame themselves for the traumatic birth. They can also block out many memories of the birth experience.
After dealing with all this, many women become extremely fearful of getting pregnant again and having to experience childbirth in the future.

What is a traumatic birth?
Most women spend time imagining what their birth experience will be like, regardless of whether it is their first birth. When their birth experience is different from what they imagine, women experience psychological distress. How women (and people at their delivery) react to and process the event determines the degree of trauma.
When the reality of the birth, or events leading up to or immediately following, is vastly different from what was hoped for, women can go through a whole range of difficult emotions. -Dr. Sarah Allen
When a C-section or another intervention becomes an emergency, medical staff are less likely to communicate with the mom about what is happening. Things start happening very quickly, leaving her feeling powerless, afraid, and disembodied.
A surreal experience
Ellen S., a mother of two children, had an extremely traumatic birth of her first child. At the time of her delivery, she only remembers her midwife telling her that the only way to deliver her baby safely, vaginally, would be with forceps. She learned the one doctor “left on the planet who could still use forceps happened to be in the hospital that night.” Ellen could choose to try a forceps delivery (the risks of which she knew nothing about) or have a C-section. She needed to decide immediately because her baby’s heart rate was dangerously low, and his life was in danger.
Ultimately, she chose forceps, but only because she had been committed to trying to have a vaginal delivery. Luckily both she and her son survived the delivery. Unfortunately, she sustained a severe pelvic tear and major bleeding that sent her to the operating room after her delivery. In her words:
The whole thing was bizarre, surreal. But the physical trauma was real. -Ellen S., Birth Trauma survivor
Experiencing sanctuary trauma
Very often, the fact that the result of the traumatic birth is a healthy baby robs mothers of understanding or support. In the research literature on psychological trauma, this is known as “sanctuary trauma.” Sanctuary trauma occurs when a person has experienced a traumatic event and turns to others for support. Instead of offering support, these people either ignore or dismiss the issue, further contributing to a survivor’s sense of isolation and trauma.
One of the cruelest things about birth trauma is that it’s often minimized by those surrounding the birthing person. -Lynne McIntyre, LCSW
The contrast between a mom’s lived experience of the birth and her support network’s dismissive response is devastating. It comes at a time when most new moms need love and support more than ever.
The fact that the outcome is a healthy baby – that’s the bar for success. Whatever happened to the mom along the way to that healthy baby doesn’t matter or is quickly forgotten. -Ellen S.
What puts moms at risk for emotional harm after birth trauma?
The emergency nature of medical interventions during labor can make the experience damaging and traumatic. The two most significant determinants of the emotional impact of women’s birth experience are:
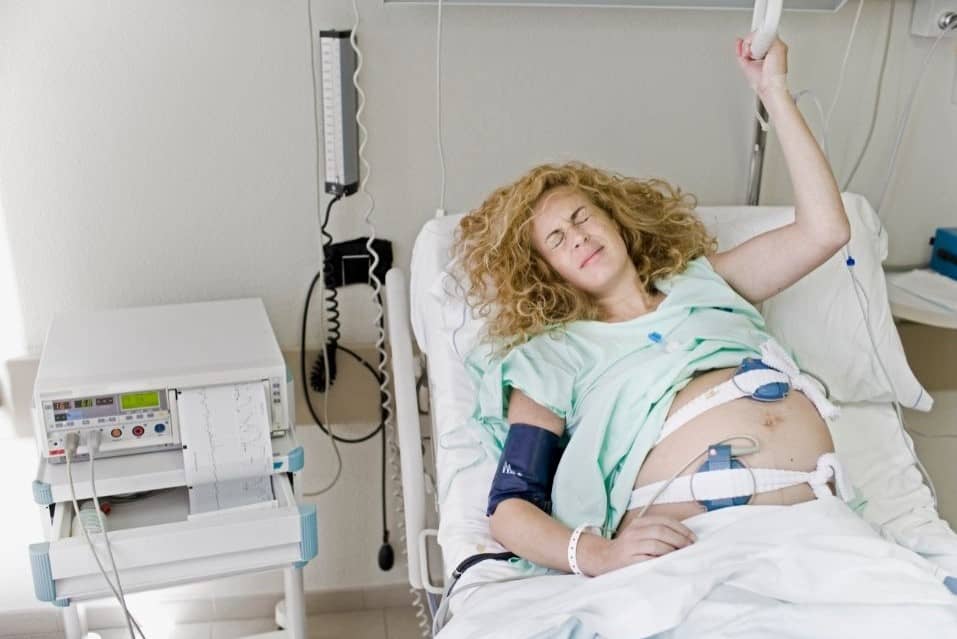
- How many interventions their birth involved. For example, electronic fetal monitoring, vacuum, vaginal lacerations, postpartum bleeding, or shoulder obstruction.
- How dissatisfied women are with their delivery experience.
Dr. Sarah Allen, psychologist and author of The Guide to Pregnancy & Postpartum Stress, Anxiety, and Depression, reports that the other major contributors to birth trauma are:
- Pain
- Previous traumatic experiences such a sexual abuse
- Feeling that at some point during the experience that everything was out of her control.
What can you do if you think you, your partner, or a friend experienced birth trauma?
If you or someone close to you had a traumatic birth, you can’t change that. But you can take positive steps towards recovering from the trauma. Though healing and recovery are not a straight line and may take many months, it is possible.
1. Talk to your (their) OB provider who was at the delivery.
It is your (their) body, and you have a right to know what happened to it and why. In addition, you can request your delivery notes from the hospital if you think it will be helpful in your healing from the event.
2. Find a moment, a pen, and a journal to write down your version of your birth.
Trauma research shows that writing helps foster healing. Your version of events and what it felt like to live through them is yours alone to tell. Storytelling can be empowering for survivors – when they are ready.
3. Find a counselor or therapist.
Look for someone experienced in working with postpartum moms and trauma survivors. Many therapists recommend EMDR (eye movement desensitization and reprocessing) for quick and effective treatment of PTSD in postpartum moms.
4. Find a support group or online mental health support platform.
Talk with women who can validate your experience and your emotions. Examples include The Birth Trauma Association and Postpartum Support International.
5. Remember you, or they, are not to blame.
There is no room for guilt or shame in birth trauma. Recognize that you did the best you could under the circumstances and with the knowledge you had at the time. If you are a partner, recognize that you may also have been traumatized and need to recover and heal as well.
6. Build your recovery team.
Get expert help and treatment for any lasting complications of the traumatic birth. These could be pain, trouble breastfeeding, problems holding urine, insomnia, relationship problems, or sexual problems.
Make yourself (or your loved one) as much of a priority as the new baby. Don’t downplay the severity of the trauma. Instead, validate the need for healing mentally and physically.
Meeting women’s mental health needs after birth trauma
There are several ways to try to prevent women from going through traumatic birth experiences. The prevention approach is to limit the amount of intrusive obstetrical interventions modern-day hospital births involve. Organizations such as PATTCH and The Birth & Trauma Support Center offer classes and resources for medical professionals to minimize birth trauma.
A second strategy is to implement a more thorough and sensitive debriefing after a traumatic birth. For example, obstetrical providers could find women at risk of PTSD based on delivery reports. They would refer them for earlier postpartum visits, preferably with the provider who performed the delivery.
Even if the birth did not go according to a family’s hopes they can be quite resilient and do quite well if they felt the process was respectful, collaborative and safe. Being able to tell their stories, have questions answered, and feel heard are all integral to beginning the healing process. -Krysta Dancy, MA and founder of The Birth & Trauma Support Center
Left in the dark
Ellen, the survivor of forceps delivery and postpartum bleeding, was frustrated and scared. “I didn’t get all the information. I didn’t know how close to death I really was.” Even with a bad laceration and having survived a severe bleeding, no one on her delivery team explained afterward what had happened.
Addressing the lack of referral to support services for women experiencing obstetrical trauma is the third strategy for reducing traumatic birth experiences. Her traumatic forceps delivery caused nerve damage to her tailbone and prevented her from standing up straight for six weeks after her delivery. Despite this, Ellen’s midwife never referred her for any pelvic floor physical therapy, regular physical therapy, or mental health support services. At her post-birth checkup, her midwife only did a perfunctory pelvic exam and reassured her that she was fine to resume sexual intercourse, the last thing from Ellen’s mind.
The call for better care
Perinatal mental illness is largely under diagnosed and under treated. High rates of obstetric intervention in many birth settings means that women need improved psychological care from health professionals to reduce the risk of traumatic childbirth. Early screening, diagnosis, and management of birth trauma should be considered a mandatory part of perinatal care.
Trauma survivors commonly distance themselves from loved ones, cannot feel loving emotions, and lose hope or excitement for the future. The impact of these emotional reactions can be devastating to mother-baby bonding. Healing birth trauma is critical for a woman and her family’s mental health. Given that the psychological effects of childbirth can be far-reaching and have long-lasting consequences for a woman and her family, women’s health providers and the health care system owe women a higher standard of care.


 Learn
Learn Get News
Get News Find Help
Find Help
 Share
Share
 Share
Share
 Share
Share
 Share
Share



